Immune-Mediated Blood Diseases in Dogs and Cats: IMHA, ITP, and What Pet Owners Need to Know
Your pet’s immune system is designed to protect them from infections and disease. But sometimes it misfires, targeting healthy blood cells as though they were invaders. When the immune system destroys red blood cells, it causes a condition called immune-mediated hemolytic anemia, or IMHA. When it destroys platelets, the cells responsible for clotting, the result is immune-mediated thrombocytopenia, or ITP. Both conditions can become life-threatening quickly, which is why recognizing the early warning signs matters so much.
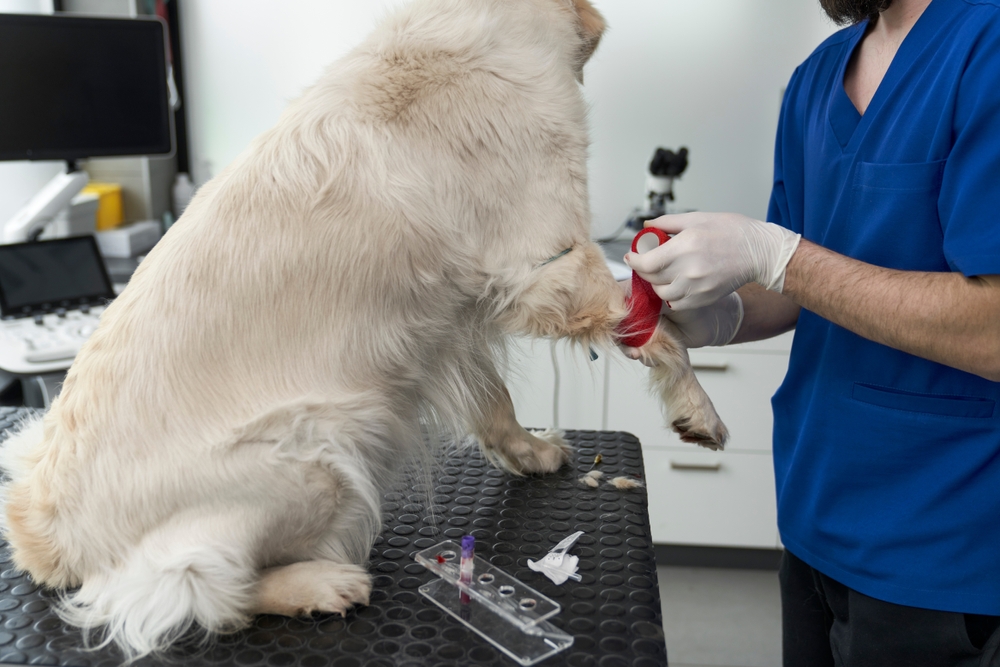
At Flora Family Vet, we are an AAHA-accredited practice with in-house diagnostics that allow us to evaluate your pet’s blood counts and start treatment the same day symptoms appear. In central Florida, where ticks are active year-round, we also screen for tick-borne infections that can trigger or mimic auto-immune blood disorders. If your pet seems unusually tired, has pale gums, or is bruising without explanation, same-day urgent care is available. Book now or contact us to have your pet seen promptly.
How the Immune System Turns on the Blood
The immune system is built to recognize and eliminate foreign invaders. Immune-mediated diseases develop when the immune system makes a critical error, marking its own red blood cells or platelets for destruction.
These conditions are classified as either primary or secondary, and that distinction shapes how we approach treatment.
Primary IMHA and ITP are idiopathic, meaning the immune attack occurs without an identifiable cause. These cases are treated by suppressing the immune response directly.
Secondary IMHA and ITP occur when something triggers the immune attack: an infection, toxin, drug, cancer, or envenomation. In these cases, treating the underlying cause is just as important as managing the immune response, and without addressing the trigger, the condition tends to relapse or fail to resolve fully.
IMHA: When Red Blood Cells Are the Target
Recognizing the Signs Before a Crisis
Immune-mediated hemolytic anemia occurs when antibodies attach to red blood cells and mark them for destruction. As those cells are eliminated faster than the bone marrow can replace them, oxygen delivery to every organ in the body becomes progressively compromised.
Early and escalating signs of IMHA:
- Unusual fatigue or withdrawal from normal activity
- Faster breathing than normal, even when resting
- Pale or jaundiced gums (yellow coloring from bilirubin released by destroyed red cells)
- Dark brownish or port-wine colored urine from hemoglobin being filtered through the kidneys
- Loss of appetite, sometimes even for foods your pet loves
Some breeds have a documented breed predisposition to IMHA. American Cocker Spaniels, Irish Setters, and several others develop this condition at higher rates, making early sign recognition particularly valuable for families with these breeds.
Secondary Causes of IMHA: What Might Be Behind It
When IMHA is secondary, something identifiable set off the immune attack. The list of potential triggers is broader than many people expect.
Infectious triggers:
- Tick-borne diseases: Ehrlichia, Anaplasma, Rocky Mountain spotted fever, and Babesia (a parasite that directly invades red blood cells while simultaneously triggering immune destruction) are all active in central Florida year-round
- Leptospirosis: a bacterial infection spread through water and soil contaminated by infected wildlife urine; particularly relevant in Florida’s wet environment and a potential trigger for both IMHA and ITP
- Hemotropic Mycoplasma: primarily in cats- bacterial parasites that attach to the surface of red blood cells and trigger immune-mediated destruction; transmitted by fleas and ticks
Cancers that can trigger IMHA:
- Lymphoma: one of the most common cancers in dogs; can produce IMHA as a paraneoplastic effect (a condition caused by the body’s immune response to cancer rather than the tumor directly)
- Feline leukemia virus: FeLV can cause anemia through several mechanisms, including immune-mediated red blood cell destruction
- Hemangiosarcoma: an aggressive cancer of blood vessel walls that causes hemolytic anemia both mechanically and through immune activation
Toxin exposure:
- Zinc toxicosis: zinc from pennies minted after 1982, certain hardware items, or zinc-containing supplements directly damages red blood cell membranes and triggers hemolytic anemia; a surprisingly common accidental toxicity in dogs
- Onions and garlic: both contain compounds that oxidize red blood cells and cause hemolytic anemia in dogs and cats; cooked and powdered forms are more dangerous than raw, and cats are significantly more sensitive than dogs
Drugs and envenomations:
- Certain antibiotics, particularly sulfonamides, can trigger immune-mediated blood cell destruction in susceptible individuals
- Snake bites: venom from venomous species can cause direct red blood cell breakdown as well as coagulation disorders that overlap with IMHA presentation
- Bee stings and insect venoms can provoke acute hemolytic reactions in sensitized individuals
The Clotting Paradox in IMHA
Here is what makes IMHA especially dangerous: while the immune system destroys red blood cells, the clotting system simultaneously becomes dysregulated. Rather than bleeding freely, the body paradoxically forms abnormal clots in the lungs, abdomen, or limbs. Blood clotting complications are among the leading causes of death in IMHA and are the primary reason hospitalization and close monitoring matter so much.
Signs of a possible clot requiring immediate care:
- Sudden difficulty breathing
- A limb that is cold, painful, or swollen compared to the others
- Collapse or acute severe weakness
Call us immediately or proceed to the nearest emergency facility if these signs appear. Our urgent care is available during open hours.
ITP: When Platelets Are Under Attack
Immune-mediated thrombocytopenia targets platelets rather than red blood cells. Platelets are responsible for initiating clot formation at sites of injury, and when their numbers fall below a critical level, bleeding becomes difficult to control and can occur without obvious trauma.
Signs that suggest ITP:
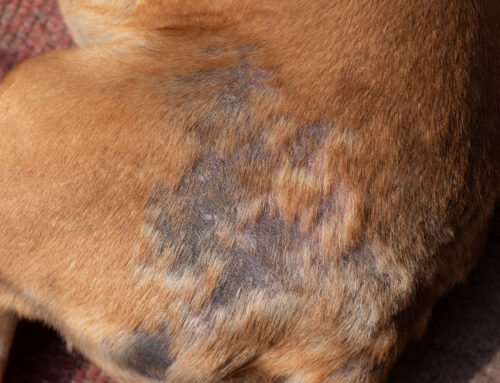
- Unexplained bruising, especially on the belly, inner thighs, or gums
- Petechiae: tiny pinpoint red or purple dots on the skin or inside the mouth
- Nosebleeds with no obvious injury
- Blood in the urine or stool
- Wounds or minor cuts that bleed disproportionately long
ITP can cause internal bleeding with no external sign at all. A pet with only mild-looking bruises may be hemorrhaging internally.
What Can Trigger ITP
Like IMHA, ITP can be primary (immune system error without a known cause) or secondary to an underlying condition. Triggers include:
- Tick-borne infections: Ehrlichia in particular can produce platelet destruction that is clinically indistinguishable from primary ITP without specific testing
- Heartworm disease: chronic infection can deplete platelets as the clotting system responds to vessel and tissue damage caused by the parasites
- Canine distemper virus: can trigger platelet destruction as part of its systemic effects
- Leptospirosis: severe bacterial leptospirosis infection can cause thrombocytopenia alongside its effects on the kidneys and liver
- Medications: sulfonamide antibiotics are the most frequently implicated drug class; certain other medications have also been associated with immune-mediated platelet destruction
- Cancers: lymphoma and other malignancies can produce ITP as a paraneoplastic effect, just as they can with IMHA
- Vaccines: rarely, vaccination has been temporally associated with ITP onset; this is uncommon and the benefits of vaccination far outweigh the risk, but worth mentioning to us if signs develop within a few weeks of a vaccine
Evans Syndrome: Simultaneous Attack on Both
Some pets develop concurrent immune-mediated conditions affecting both red blood cells and platelets simultaneously. This combination is called Evans syndrome, and it requires treatment addressing both components at once. Managing one while ignoring the other can make the overall situation worse, and these cases require intensive monitoring and frequent medication adjustments.
Florida’s Tick Problem
In central Florida, ticks are not a seasonal concern; they are a year-round reality. This matters directly for IMHA and ITP because several tick-borne infections can trigger or precisely mimic these immune-mediated blood disorders.
Tick-borne diseases relevant to blood disorders in Florida:
- Lyme disease: can trigger immune reactions affecting blood and joint health
- Rocky Mountain spotted fever: causes serious blood vessel and platelet damage; prevalent in Florida
- Ehrlichia and Anaplasma: both target white blood cells and platelets; ehrlichiosis can be clinically indistinguishable from primary ITP without a tick panel
- IMHA secondary to Babesia: Babesia parasites invade red blood cells and trigger immune-mediated destruction at the same time
This is why tick-borne disease testing is standard in our workup for any suspected immune-mediated blood disorder. Treating what appears to be primary IMHA or ITP without ruling out an infectious driver can lead to incomplete treatment and relapse.
What the Diagnostic Workup Involves
When a pet arrives with signs of a blood disorder, we move quickly. Here is what the evaluation typically includes:
- Take a thorough history: tick exposure, known medications, when symptoms started, how rapidly they developed, any known toxin exposure or envenomation
- Perform a physical exam: gum color, heart and lung sounds, body condition, signs of bruising or petechiae
- Run a complete blood count and blood smear: quantifies red blood cells, white blood cells, and platelets; microscopic examination reveals agglutination (clumped red cells) and spherocytes (signs of immune-mediated destruction)
- Perform a Coombs test: detects antibodies bound to red blood cell surfaces, confirming immune-mediated destruction
- Check a reticulocyte count: measures whether the bone marrow is generating new red blood cells in response to the loss
- Run a chemistry panel: evaluates kidney and liver function to guide safe medication choices
- Screen for tick-borne diseases: panels for the major tick-transmitted infections active in Florida year-round
- Evaluate for underlying cancer or toxin exposure: when secondary causes are suspected based on history or initial findings
Our in-house diagnostics deliver same-day results for most panels, allowing treatment to begin the same visit.
Treatment: Stopping the Attack, Supporting the Body
Treatment has two parallel goals: stopping the immune system from continuing to destroy blood cells, and supporting the pet’s body while counts recover. For secondary IMHA and ITP, treating the underlying trigger is equally important. Immune-mediated disease treatment is individualized and continuously adjusted; some dogs and cats require maintenance therapy long-term.
IMHA Treatment
- Corticosteroids (prednisolone): the cornerstone of immunosuppressive therapy; slows or stops the immune attack on red blood cells
- Additional immunosuppressants: added when steroid response is inadequate or when a more aggressive approach is needed from the outset
- Anti-clotting medications: for patients at high thrombosis risk based on blood work patterns
- Supportive care: IV fluids, oxygen supplementation, stomach protectants for steroid-related gastrointestinal effects
- Blood transfusions: sometimes necessary to stabilize severely anemic patients while immunosuppression takes effect
- Therapeutic plasma exchange (TPE): an emerging treatment that filters the antibodies responsible for red blood cell destruction directly out of the bloodstream; this blood purification process is used in severe or refractory cases and can buy critical time for other treatments to take effect
- Targeted antimicrobials: when a tick-borne organism, leptospirosis, or hemotropic mycoplasma is confirmed as the underlying trigger
ITP Treatment
- Corticosteroids: first-line treatment to suppress the immune attack on platelets
- Vincristine: a chemotherapy agent used at very low doses specifically to boost platelet release from the bone marrow and modulate the immune response; often added early in severe cases to bring platelet counts up faster
- Intravenous immunoglobulin (IVIG): infusions of antibody proteins that temporarily block the immune system’s ability to destroy platelets; used when platelet counts are critically low or when standard therapy is not working fast enough
- Splenectomy: surgical removal of the spleen in refractory cases where it is the primary site of platelet destruction; not first-line treatment but can produce durable remission in select patients
Tick Prevention Is Direct Prevention
Because Florida’s tick population creates year-round exposure risk, consistent tick prevention directly reduces the risk of secondary blood disorders triggered by tick-borne infections. Gaps in prevention create windows that can be exploited.
Tick prevention through veterinarian-recommended prescription products is significantly more reliable than over-the-counter options. Year-round use is the appropriate standard for pets in Florida. Our wellness and prevention team can help select the right protocol based on your pet’s lifestyle and exposure profile.
Warning Signs That Need Urgent Attention
Do not wait for a scheduled appointment if your pet shows:
- Sudden weakness, stumbling, or collapse
- Pale, white, or yellowish gums
- Unexplained bruising or petechiae on the skin or gums
- Rapid or labored breathing at rest
- Dark, discolored, or blood-tinged urine
- Significant lethargy that prevents normal rising or activity
Same-day urgent care in Kissimmee is available at Flora Family Vet for these presentations. Call ahead if possible so we can prepare for your arrival.
Frequently Asked Questions
What is the difference between primary and secondary IMHA or ITP?
Primary means the immune system attacked blood cells without an identifiable underlying cause. Secondary means something triggered the attack: an infection, toxin, drug, cancer, or venom. The distinction matters because secondary cases require treating the trigger, not just suppressing the immune response.
What is the difference between IMHA and ITP?
IMHA destroys red blood cells, reducing oxygen delivery and causing pale gums, fatigue, and labored breathing. ITP destroys platelets, impairing clotting and causing bruising, bleeding, and petechiae. Both are serious, both are treatable, and some pets develop both simultaneously (Evans syndrome).
Can these conditions recur after treatment?
Yes. Relapses occur, which is why monitoring blood counts through scheduled rechecks is important even after your pet appears to have fully recovered.
How long does recovery take?
Initial stabilization typically takes days to weeks. Full medication tapering may take months. Some pets require ongoing low-dose maintenance therapy to prevent relapse.
Moving from Uncertainty to a Plan
An immune-mediated blood disease diagnosis is frightening, but it is also a condition where fast, accurate diagnosis and appropriately aggressive treatment give most pets a genuine chance at recovery. The families who do best are those who recognize the warning signs early and act on them.
At Flora Family Vet, our AAHA-accredited team, same-day urgent care capability, and in-house diagnostics are built for exactly this kind of time-sensitive situation. Book now or contact us if your pet is showing any of the signs above. We treat your family like ours.





Leave A Comment